1800 Calorie Ada Diet Principles Of Art HarmonyCalories Diets . Exercise is not mentioned in the plan. In any case, if you need to lose up to 1. Day Diet might be for you. Surprisingly surviving the test of time, the 3 Day Diet is dating back to 1. However, no diet book exists to substantiate the science behind the . Instead of regular price of $5 get it now for $1 only.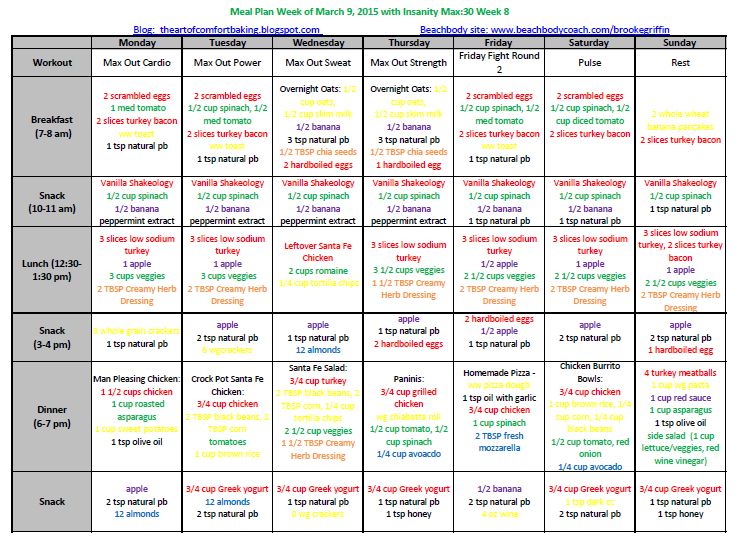  
Limited time sale. Please always consult with your doctor before starting any diet , including the ones offered in this app. This app should be helpful for those who count calories ,want a meal regiment that is under 1. Or even those who want to try famous 3- day diet. Diese App bietet Ihnen mit 1.  
1800 Calorie Ada Diet Principles Of Art ExamplesKalorien Di. Es besteht jedoch keine Di. Begrenzte Zeit verkaufen. Bitte immer mit Ihrem Arzt vor Beginn einer Di.

Reference. com. Q: Why is the website down? A: Great question! We are very sorry for any inconvenience. In the meantime, please refresh this page to try again or go to home page. 1800 Calorie Week 1 Recipe Meal Plan. Learn about the diabetic diet and how to count carbs. 1,800 Calorie ADA Diet: Also known as the Carb Consistent Diet. On a typical 1,800 Calorie diet. Meal Planning Guide 1800 Calorie. American Diabetes Association and American Dietetic Association, 2007. 1800 CALORIE MEAL PLAN. 
Nutrition Principles and Recommendations in Diabetes. Medical nutrition therapy is an integral component of diabetes management and of diabetes self- management education. Yet many misconceptions exist concerning nutrition and diabetes. Moreover, in clinical practice, nutrition recommendations that have little or no supporting evidence have been and are still being given to persons with diabetes. Accordingly, this position statement provides evidence- based principles and recommendations for diabetes medical nutrition therapy. The rationale for this position statement is discussed in the American Diabetes Association technical review “Evidence- Based Nutrition Principles and Recommendations for the Treatment and Prevention of Diabetes and Related Complications,” which discusses in detail the published research for each principle and recommendation (1). Historically, nutrition recommendations for diabetes and related complications were based on scientific knowledge, clinical experience, and expert consensus; however, it was often difficult to discern the level of evidence used to construct the recommendations. To address this problem, the 2. American Diabetes Association evidence grading system. However, the best available evidence must still take into account individual circumstances, preferences, and cultural and ethnic preferences, and the person with diabetes should be involved in the decision- making process. The goal of evidence- based recommendations is to improve diabetes care by increasing the awareness of clinicians and persons with diabetes about beneficial nutrition therapies. Because of the complexity of nutrition issues, it is recommended that a registered dietitian, knowledgeable and skilled in implementing nutrition therapy into diabetes management and education, be the team member providing medical nutrition therapy. However, it is essential that all team members be knowledgeable about nutrition therapy and supportive of the person with diabetes who needs to make lifestyle changes. GOALS OF MEDICAL NUTRITION THERAPY FOR DIABETESGoals of medical nutrition therapy that apply to all persons with diabetes are as follows: Attain and maintain optimal metabolic outcomes including. Blood glucose levels in the normal range or as close to normal as is safely possible to prevent or reduce the risk for complications of diabetes. A lipid and lipoprotein profile that reduces the risk for macrovascular disease. Blood pressure levels that reduce the risk for vascular disease. Prevent and treat the chronic complications of diabetes. Modify nutrient intake and lifestyle as appropriate for the prevention and treatment of obesity, dyslipidemia, cardiovascular disease, hypertension, and nephropathy. Improve health through healthy food choices and physical activity. Address individual nutritional needs taking into consideration personal and cultural preferences and lifestyle while respecting the individual’s wishes and willingness to change. Goals of medical nutrition therapy that apply to specific situations include the following: For youth with type 1 diabetes, to provide adequate energy to ensure normal growth and development, integrate insulin regimens into usual eating and physical activity habits. For youth with type 2 diabetes, to facilitate changes in eating and physical activity habits that reduce insulin resistance and improve metabolic status. For pregnant and lactating women, to provide adequate energy and nutrients needed for optimal outcomes. For older adults, to provide for the nutritional and psychosocial needs of an aging individual. For individuals treated with insulin or insulin secretagogues, to provide self- management education for treatment (and prevention) of hypoglycemia, acute illnesses, and exercise- related blood glucose problems. For individuals at risk for diabetes, to decrease risk by encouraging physical activity and promoting food choices that facilitate moderate weight loss or at least prevent weight gain. MEDICAL NUTRITION THERAPY FOR TYPE 1 AND TYPE 2 DIABETESCarbohydrate and diabetes. When referring to common food carbohydrates, the following terms are preferred: sugars, starch, and fiber. Terms such as simple sugars, complex carbohydrates, and fast- acting carbohydrates are not well defined and should be avoided. Studies in healthy subjects and those at risk for type 2 diabetes support the importance of including foods containing carbohydrate, particularly from whole grains, fruits, vegetables, and low- fat milk in the diet of people with diabetes. A number of factors influence glycemic responses to foods, including the amount of carbohydrate, type of sugar (glucose, fructose, sucrose, lactose), nature of the starch (amylose, amylopectin, resistant starch), cooking and food processing (degree of starch gelantinization, particle size, cellular form), and food form, as well as other food components (fat and natural substances that slow digestion—lectins, phytates, tannins, and starch- protein and starch- lipid combinations). Fasting and preprandial glucose concentrations, the severity of glucose intolerance, and the second meal or lente effect of carbohydrate are other factors affecting the glycemic response to foods. However, in persons with type 1 or type 2 diabetes, ingestion of a variety of starches or sucrose, both acutely and for up to 6 weeks, produced no significant differences in glycemic response if the amount of carbohydrate was similar. Studies in controlled settings and studies in free- living subjects produced similar results. Therefore, the total amount of carbohydrate in meals and snacks will be more important than the source or the type. Studies in subjects with type 1 diabetes show a strong relationship between the premeal insulin dose and the postprandial response to the total carbohydrate content of the meal. Therefore, the premeal insulin doses should be adjusted for the carbohydrate content of the meal. For individuals receiving fixed doses of insulin, day- to- day consistency in the amount of carbohydrate is important. In persons with type 2 diabetes, on weight maintenance diets, replacing carbohydrate with monounsaturated fat reduces postprandial glycemia and triglyceridemia. However, there is concern that increased fat intake in ad libitum diets may promote weight gain. Therefore, the contributions of carbohydrate and monounsaturated fat to energy intake should be individualized based on nutrition assessment, metabolic profiles, and treatment goals. Glycemic index. Although low glycemic index diets may reduce postprandial glycemia, the ability of individuals to maintain these diets long- term (and therefore achieve glycemic benefit) has not been established. The available studies in persons with type 1 diabetes in which low glycemic index diets were compared with high glycemic index diets (study length from 1. In subjects with type 2 diabetes, studies of 2–1. Hb. A1c, fructosamine, or insulin levels. The effects on lipids from low glycemic index diets compared with high glycemic index diets are mixed. Although it is clear that carbohydrates do have differing glycemic responses, the data reveal no clear trend in outcome benefits. If there are long- term effects on glycemia and lipids, these effects appear to be modest. Moreover, the number of studies is limited, and the design and implementation of several of these studies are subject to criticism. Fiber. As for the general population, people with diabetes are encouraged to choose a variety of fiber- containing foods, such as whole grains, fruits, and vegetables, because they provide vitamins, minerals, fiber, and other substances important for good health. Early short- term studies using large amounts of fiber in small numbers of subjects with type 1 diabetes suggested a positive effect on glycemia. Recent studies have reported mixed effects on glycemia and lipids. In subjects with type 2 diabetes, it appears that ingestion of very large amounts of fiber are necessary to confer metabolic benefits on glycemic control, hyperinsulinemia, and plasma lipids. It is not clear whether the palatability and the gastro- intestinal side effects of fiber in this amount would be acceptable to most people. Sweeteners. The available evidence from clinical studies demonstrates that dietary sucrose does not increase glycemia more than isocaloric amounts of starch. Thus, intake of sucrose and sucrose- containing foods by people with diabetes does not need to be restricted because of concern about aggravating hyperglycemia. Sucrose should be substituted for other carbohydrate sources in the food/meal plan or, if added to the food/meal plan, adequately covered with insulin or another glucose- lowering medication. Additionally, intake of other nutrients ingested with sucrose, such as fat, need to be taken into account. In subjects with diabetes, fructose produces a lower postprandial response when it replaces sucrose or starch in the diet; however, this benefit is tempered by concern that fructose may adversely effect plasma lipids. Therefore, the use of added fructose as a sweetening agent is not recommended; however, there is no reason to recommend that people with diabetes avoid naturally occurring fructose in fruits, vegetables, and other foods. Sugar alcohols produce a lower postprandial glucose response than fructose, sucrose, or glucose and have lower available energy values. However, there is no evidence that the amounts likely to be consumed in a meal or day result in a significant reduction in total daily energy intake or improvement in long- term glycemia. The use of sugar alcohols appears to be safe; however, they may cause diarrhea, especially in children. The Food and Drug Administration has approved four non- nutritive sweeteners for use in the U. S.—saccharin, aspartame, acesulfame potassium, and sucralose.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. Archives
November 2017
Categories |
 RSS Feed
RSS Feed
